Nursing PhD graduate creates toolkit to improve communication for ICU patients

Laura Istanboulian, a new graduate of the Lawrence S. Bloomberg Faculty of Nursing, created a “communication bundle” to help solve a decades-old problem in hospital ICUs (supplied photo)
Published: June 6, 2023
Already juggling a career as a nurse practitioner, marriage, two kids and aging parents, Laura Istanboulian wondered if she was too old – or if it was too late – to pursue her doctorate in nursing science.
Yet it had been her dream to complete her PhD – and as a nurse, she was motivated to situate her research around her patients. She was specifically interested in addressing a decades-old problem in hospital intensive care units (ICUs) that makes it difficult for individuals who require a ventilator to communicate with their health-care providers.
Istanboulian decided to pursue her doctorate, making it her objective to reframe communication as something essential to a quality patient experience.
While in the program, she co-designed and implemented a bundled communication toolkit for ICU patients as part of her PhD at the Lawrence S. Bloomberg Faculty of Nursing.
The bundle is a portable, multi-modal set of tools that Istanboulian co-designed with nurses, patients and their families. Each item in the bundle is evidence-based in supporting the communication needs of patients – including alphabet boards, blank boards for writing on, writing tools like markers and pencils, a pain scale, a basic needs scale and some pre-translated boards in multiple languages.
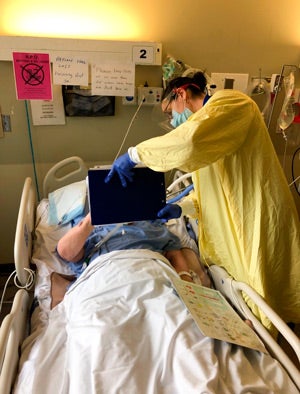
The bundle also contains six short education modules for staff to gain a better understanding of how to use each tool option to best support a patient.
“I was not trying to invent something brand-new – these tools existed already, but it became necessary to have them contained in one convenient and accessible location, and to also make providers aware of the need to make an effort to communicate with ventilated patients,” Istanboulian explains.
When a patient is on a ventilator, no air can pass over their vocal cords – meaning that they cannot speak. They might make efforts to communicate – but that requires both interpretation and time from the health-care provider, which is not always available, Istanboulian says.
Some patients may also have cognitive impairments or brain dysfunction from their illness or medical condition, making communication that much harder – and their fear from not knowing what is going on even more palpable.
Istanboulian notes that limited communication with a patient can also affect care providers.
“It can be intimidating caring for someone when you cannot explain what it is happening to them or understand what they are trying to say,” she says.
Istanboulian recounts a moment when she used the new communication tools to try to understand one of her clients, who could not speak or hear.
“On the blank board, he wrote, ‘Thank you so much for taking the time.’ I took a photo of that and it hangs by my desk, because it is a reminder that this effort to communicate really mattered to this person – and it also tells me that this doesn’t happen as a rule,” she says.
“As nurses and physicians, we might be doing the best for them medically, but if patients don’t understand what is happening to them, they can feel very unsafe and alone.”
Developing the communication bundle was not without its challenges, especially as Istanboulian began her PhD just as the COVID-19 pandemic began to unfold.

“Laura overcame significant obstacles posed by the global pandemic to complete her doctoral research,” says Istanboulian’s supervisor Craig Dale, an associate professor in the Lawrence S. Bloomberg Faculty of Nursing.
“She designed, implemented and evaluated this communication-support intervention for mechanically ventilated adult patients in the ICU and the outcome of her research has the potential to be implemented in ICUs worldwide – a positive impact that extends well beyond the pandemic.”
Despite the constantly shifting policies around visitors and isolation requirements for the ICU, Istanboulian found most families, patients and nurses were more than willing to help her design the new tools.
“They really wanted to engage in this process – which was so profound to me, because it showed how much everyone wanted to see this issue of communication addressed,” Istanboulian says.
Families and caregivers offered helpful tips for nurses on providing phone updates on loved ones, and nurses were able to speak to what they would find most helpful in using the bundle, including how to easily share some of the online tools using the internal hospital intranet.
Following the initial success of the tools, Istanboulian is keen to scale up the bundle so that it is accessible to larger units in the hospital – and eventually available across multiple hospital sites within the health-care system.
Istanboulian says one of the key lessons she learned from the project was that the toolkit does require tailoring to local environments in order to meet the needs of the end users. She is currently working with an international group of researchers who are developing core outcomes for communications research in critical care and recommendations that will assist in scaling up the bundle.
Her work with researcher Dr. Kelly Smith – a specialist in health-care quality and patient safety who is an associate professor and co-lead for outcomes and evaluation at U of T's Institute of Health Policy, Management & Evaluation – will also help to determine how patients and family members interpret communication as a safety issue and help reframe communication as something that many see as simply "nice to have," Istaboulian says, to something essential to a patient's experience.
As Istanboulian embarks on life after her PhD, which includes ongoing research and a new position as an assistant professor at Toronto Metropolitan University, she's grateful for the many people that helped her on her path to graduating with her doctorate.
“My wife was my No. 1 – she was always making space for me to be able to write or research. My supervisor and clinical supervisor were so supportive of me not only conducting the research, but maintaining my clinical practice; and my parents were so proud of me,” Istanboulian says.
“I’m not sure everyone is as fortunate to have that level of support – and I think that was really the recipe for this dream becoming a reality.”



