Male physicians refer patients to male surgeons at disproportionate rates: U of T study

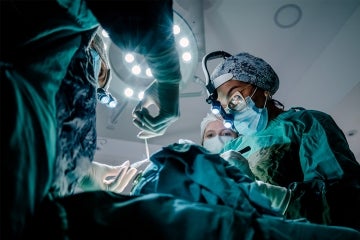
(Photo by Morsa Images via Getty Images)
Published: November 11, 2021
A study that analyzed nearly 40 million referrals to surgeons in Ontario found male physicians disproportionately refer patients to male surgeons over similarly qualified and experienced female surgeons.
The study, published this week in JAMA Surgery, showed that the differences in referral volumes and types could not be explained by patients’ choices or by characteristics of the surgeon, including age or experience.
The findings suggest that male physicians hold biases that disadvantage female surgeons, further widening the gender pay gap in medicine.
“During my 20 years in practice, I always had the sense it was easier for my male surgical colleagues to get referrals than it was for me, and the patients they were referred were more likely to need surgery,” said Nancy Baxter, senior author on the study.
“Our work demonstrates that my observations were not unique but reflect gender bias that affects the lives and livelihoods of all female surgeons in the province.”
A professor of surgery at the University of Toronto’s Temerty Faculty of Medicine. Baxter is also affiliated with the Institute of Health Policy, Management and Evaluation at the Dalla Lana School of Public Health and St. Michael’s Hospital at Unity Health Toronto.
The researchers compared the proportion of referrals made by male and female physicians to male and female surgeons over a 10-year span from 1997 to 2016. Nearly 40 million referrals were made to 5,660 surgeons. Although male surgeons accounted for 77.5 per cent of all surgeons, they received 79 per cent of referrals sent by female physicians – and 87 per cent of referrals sent by male physicians.
The study found female physicians were 1.6 per cent likelier to refer patients to a female surgeon. Male physicians, meanwhile, were 32 per cent likelier to refer patients to a male surgeon. The differences were greatest in surgical specialties with the highest representation of female surgeons, including gynecology and plastic surgery.
Moreover, that gap remained as more women entered surgery over the study’s 10-year span.
“There is an often-made assumption that sex-based inequities in medicine will naturally improve as more women enter medicine and acquire experience,” said Fahima Dossa, co-lead author of the study and a general surgery resident based at St. Michael’s Hospital. “In contrast, our study demonstrates that inequities will not improve without active intervention – the specialties with the greatest representation of female surgeons, for example gynecology, exhibited the greatest degree of referral disparities.”
The authors say the findings demonstrate the need for efforts directly focused on eliminating sex-based biases within medicine. Dossa suggests innovative changes to the referral process, such as a single-entry referral model, in which referrals are scheduled to be seen by the first surgeon available.
The research builds on previous work by Baxter and Dossa that found female surgeons in Ontario earn 24 per cent less per hour while operating compared to male surgeons, and that female surgeons performed fewer of the highest-paid primary procedures than male surgeons.
“The time is now ripe to enact change,” Dossa said. “Our work points toward a mechanism that directly contributes to the sex-based pay gap in medicine. Focused efforts at reducing the effects of implicit and explicit biases on referrals to physicians are now needed.”
This work included researchers at the independent, non-profit research institute ICES, and was funded by the Canadian Institutes of Health Research and the Physicians’ Services Inc. Foundation.