U of T researchers design microfluidic device to understand how air pollution affects lungs

Edmond Young, of the Faculty of Applied Science & Engineering, and his research team have developed a microfluidic lung-on-a-chip that mimics breathing in human lungs (photo courtesy of Edmond Young)
Published: November 4, 2021
University of Toronto researchers in biomedical engineering have developed a new technology that combines a microfluidic device with a novel airflow system to mimic lung airways. The technology enables scientists and engineers to perform particle exposure experiments to examine the pathological effects of air pollutants on respiratory health.
Siwan Park, a PhD candidate at the Institute of Biomedical Engineering in the Faculty of Applied Science & Engineering, and Edmond Young, an associate professor in the department of mechanical and industrial engineering, recently published their findings in Advanced Materials Technologies.
The microfluidic device-on-a-chip – known as E-FLOAT, short for Extractable Floating Liquid gel-based Organ-on-a-chip for Airway Tissue modelling under airflow – is an easily modifiable system where scientists can grow lung cells in a suspended hydrogel that resembles lung tissue.
The researchers developed the device by micro-milling and bonding layers of thermoplastic. It incorporates a special channel geometry for growing the cells. An airflow system connected to the device can generate various flow rates of warm and humidified air to simulate human breathing.
“We showed that lung airway tissue can be micro-engineered in the lab, exposed to various environmental conditions, including airflow and pollutants, and then be extracted for further interrogation as if it were a real lung tissue sample,” Young says.
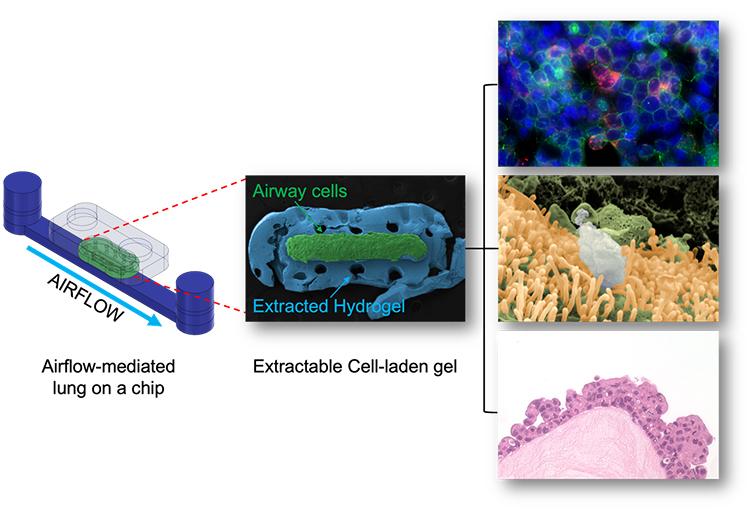
In the E-FLOAT device, lung cells are suspended in a hydrogel to mimic how they would grow in normal lung tissue. The microfluidic devices simulate breathing and exposure to air pollutants (images courtesy Siwan Park and Edmond W. K. Young)
In many existing iterations of the technology, cells grown on microfluidic devices are limited to ‘on-chip’ analysis to assess the effect of external stimuli, such as airflow, on the health of the cells. This limits the analysis that can be carried out: while scientists can remove these cells from the device, this process changes the spatial location of the cells in relationship to the tissue, potentially skewing the results.
“One of the advantages of E-FLOAT is the ability to extract the biomimetic airway tissue that allows us to develop an in-depth knowledge through a wide array of imaging technologies,” Park says.
The researchers successfully delivered airborne particles onto the airway cells via controlled airflow to mimic how air pollutants would interact with lung cells. They then extracted the entire hydrogel and analyzed particulate and cell interactions.
“We were especially excited to obtain the stunning images of histology sections using the extracted hydrogel. Not only does it look beautiful, we believe that it may also be significant in histological and pathological perspectives. Also, depending on how we design the cell-matrix interactions in E-FLOAT, we may obtain a more physiologically accurate representation of multicellular airway tissue.”
“In the future, the plan is to use this technology to study the development of lung diseases like asthma – especially in the presence of air pollution – and to also use it as a preclinical model during drug development,” Young says.
“There is obviously a lot more work to be done, but we hope to collaborate with lung researchers and partner with pharma down the road to realize this plan.”



