Researchers create “black box” for use in operating rooms to improve patient care
Published: July 8, 2014
Associate Professor Teodor Grantcharov and his team of researchers have developed a “black box” for using in operating rooms, similar to that used in the airline industry.
Dr. Grantcharov said the goal is to improve patient safety and outcomes by identifying where errors occur in the OR and teaching surgeons how to prevent them. He said that when black boxes were introduced in the aviation industry, preventable errors dropped significantly.
Grantcharov has been testing the prototype of his black box for about a month in the operating rooms at St. Michael’s Hospital, where he specializes in advanced minimally invasive surgeries, such as gastric bypasses. It’s also being tested at two hospitals in Copenhagen, Denmark, with more international sites to be involved soon.
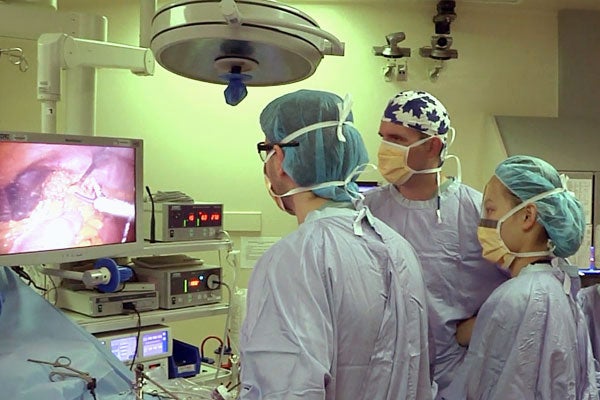
 The device (pictured at right) is about the size of a box of tissues or a thick book and it records almost everything that goes on in the OR, such as video of the surgical procedure, conversations among health care workers, room temperature and decibel levels. It works only for laparoscopic or minimally invasive surgeries that insert video cameras in thin plastic tubes into small incisions in the body that allow the surgeon to see what’s going on inside the patient.
The device (pictured at right) is about the size of a box of tissues or a thick book and it records almost everything that goes on in the OR, such as video of the surgical procedure, conversations among health care workers, room temperature and decibel levels. It works only for laparoscopic or minimally invasive surgeries that insert video cameras in thin plastic tubes into small incisions in the body that allow the surgeon to see what’s going on inside the patient.
“We want to see where errors happen in surgery so that we can understand how errors lead to adverse events and develop training curricula to prevent these errors from ever happening again,” Grantcharov said. “It doesn’t mean that we will have perfect surgeries, because we are not perfect. But it means we will learn from our errors, which will make us safer. We will train future surgeons better because we can show them what are the most critical situations and how to avoid them.”
Research has already shown that 84 per cent of errors in bypass surgery happen during the same two steps, Grantcharov said, so training has been adapted to help surgeons master those two skills. Grantcharov said he’s looking at performance issues – something the surgeon did or didn’t do, such as apply enough force when grabbing a bowel, which might make it slip and tear. But he’s also looking at less tangible factors that can lead to errors, such as communication and team dynamics.
“Say a surgeon picked up the wrong instrument. Then he got angry or frustrated and started to make technical errors. The more mistakes he made, the worse communications became.”
Grantcharov’s team has done extensive research on surgical error analysis. According to this framework, an error is a minor deviation from an optimal course of action. Errors happen during each procedure; however very few lead to adverse events and go unnoticed by the surgical team.
The landmark study on hospital medical errors in Canada, a 2004 paper by Ross Baker, a professor at the University of Toronto's Institute of Health Policy, Management and Evaluation, found that 7.5 per cent of patients admitted to acute care hospitals in Canada in 2000 experienced one or more adverse events, which can include everything from reactions to wrongly administered medications to bed sores, falls, infections and surgical errors.
Most of these events did not result in any serious harm, the study found, but almost 37 per cent were preventable. More recent studies have shown rates of adverse events in hospital between 10 and 14 per cent. Such events cost taxpayers billions of dollars, usually in longer hospital stays.
Grantcharov noted that professional athletes have coaches who point out their wrong moves and help them improve their performance.
"For surgeons, we will have data that will allow better coaching and improvements and therefore better patient care,” he said. “We will reduce the risk and complications and show how to make the OR more efficient, which will also allow us to save money and do more cases.”
Grantcharov said he also hoped his black box would bring more transparency to the OR for patients and help change the “blame-and-shame” culture that traditionally has made doctors and nurses reluctant to report mistakes.
Leslie Shepherd is a writer with St. Michael's Hospital, a partner of the University of Toronto.



