In a bid to address burnout, U of T-led study examines nurses' work environment during COVID-19
Published: May 2, 2022
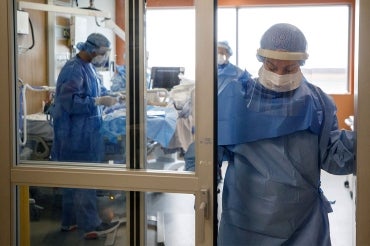
Exhausted and burned out, many nurses are leaving the workforce amid an unrelenting surge in care demands over the past two years due to the COVID-19 pandemic.
Linda McGillis Hall, a professor in the Lawrence S. Bloomberg Faculty of Nursing and a renowned international researcher with expertise in the nursing work environment, says that what is happening to nurses right now is not just a challenge, but a crisis – and one that needs to be addressed.
 Linda McGillis Hall
Linda McGillis Hall“Nurses have dealt with surges in patient care before,” says McGillis Hall. “This happened during SARS in 2003, and with hallway medicine in 2019. The difference is that those periods of surge ended – there was a reprieve.
“COVID-19 has been relentless, not providing any breaks – and with each new wave, nurses are faced with another set of care challenges causing them to reach their breaking point.”
McGillis Hall has received a grant from the Canadian Institutes of Health Research (CIHR) to learn directly from nurses across the country about what is needed to improve the nursing work environment. Along with her team of researchers from universities across Canada, the study aims to obtain a snapshot of the state of the current nursing workforce after working through so many waves of the virus and highlight ways of reducing burnout and improving the retention of nurses.
“We know from recent research about the psycho-social impacts of the pandemic on nurses, resulting in fatigue and burnout, but we don’t yet have evidence-based strategies for ways to address these impacts and mitigate them,” McGillis Hall says.
Staff shortages, along with heavier work assignments and increased patient care needs, appear to be contributing factors to the burnout nurses are currently facing. It has become exceedingly difficult for nurses to maintain a standard of care for each patient in an environment where they only have time for basic care needs.
“Nurses go into the profession because they care about working with people,” says McGillis Hall. “[So], when you hear words like the ‘new normal,’ maybe this needs more examination.”
Even prior to the pandemic, health-care organizations around the world from the WHO to the International Council of Nurses warned of an impending global nursing shortage.
Sheri Price, a professor at Dalhousie University and a co-investigator on this study, focused her doctoral research on nursing retention and recruitment in response to the predicted shortage. Following an unprecedented two years of upheaval across Canada’s health system during the pandemic, Price is now hoping the study will provide promising practice and policy changes to best support nurses.
“Nurses have insight into what supports they need, which is a huge piece of this study,” says Price, who received her PhD from the Lawrence S. Bloomberg Faculty of Nursing. “Nurses will have a voice and will be able to tell us not only about the problems they are encountering, but can also identify creative solutions because they are the ones on the ground doing the work.”
The researchers say now is the perfect time to be conducting this study as the persistent demands on health care are starting to ebb and public interest in the capacity of the health-care system remains high. Additionally, with the recent announcement by the federal government about a search for a national chief nursing officer, taking the time to anticipate and make changes to the workforce before another surge is essential.
“I see this project as a beacon of hope,” says Michelle Lalonde, an associate professor at the University of Ottawa, who is also a co-investigator on the study. “The public needs to see a bit of hope that things are going to improve, and that we will be able to uncover some concrete, action-focused recommendations for the nursing workforce.”
Lalonde, who also graduated from Bloomberg Nursing’s PhD program, has studied new nursing graduate transitions into the workforce, as well as the perspectives of francophone nurses, which will be an integral part of the pan-Canadian study.
Lalonde says that nurses who entered the workforce at the start of the pandemic will have a tremendous amount of knowledge about the challenges of entering the practice – knowledge that Sanja Visekruna, another co-investigator, agrees is critical for policy-makers when considering retention strategies.
“As a nurse educator, I’m always thinking about how I can support students who are entering the nursing workforce,” says Visekruna, an assistant professor at McMaster University and graduate of Bloomberg Nursing’s PhD program. “When I think of students entering the profession now, mentorship continues to be fundamental to building nursing competencies and the study will likely seek out new and evidence-focused ways to support this and nurses in different roles, which is critical for retention and the future of the nursing workforce.”
As the largest group of health-care providers, the well-being of nurses and their ability to uphold health systems across the country is paramount to societies well-being – a reason that the researchers feel more attention needs to be paid to the mental health and working conditions of nurses.
“We have needed evidence-informed policies to support nurses for a long time,” says Price. “It is imperative that we put the effort in now for the well-being of our nurses and the profession.”



